Common Ear Infection
As I said elsewhere, I remember when my children were young, they seemed to tag team us with ear infections. My youngest son, in particular, had a lot of problems with his ears which eventually led to him having grommets fitted. Common ear infections can happen in the outer or middle ear and they happen when germs such as bacteria, viruses or fungi cause swelling and irritation of your outer ear or inflammation of your middle ear. They are most common in childhood, however, they can happen at any age. Middle ear infections can be very dangerous if left untreated, and unfortunately, we hear of deaths caused by un-treated middle ear disease all too often. I wrote an article here on the pages of Know about one such instance where an un-diagnosed middle ear infection caused the death of Andrew Broadhurst in the UK. Less common infections can strike the inner ear, the cochlea and they can cause a whole shedload of trouble. So on this page, I want to give a full outline of ear infections.
Overview:
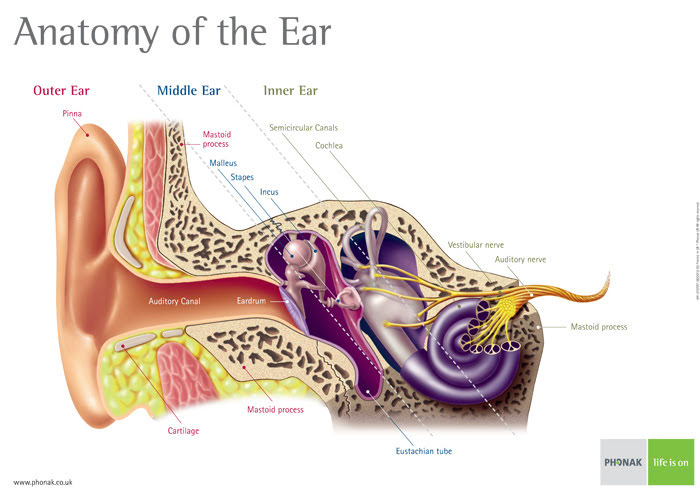
In professional terms, common infections of the ear are called by two different names based on the site of the infection. Otitis media is an infection of the middle ear and infections of the outer ear are called otitis externa. Most ear infections are uncomfortable but not serious. Many ear infections may actually clear up by themselves in a few days. In general terms, ear infections whether they are Otitis Media or Otitis Externa are unlikely to cause permanent loss or impairment of hearing but you should consult a doctor if you are getting infections often or if you have one that does not seem to be shifting. Less common inner ear infections are not normally accompanied by pain, they can induce dizziness, vomiting and a marked loss of hearing though.
Ear Pain
Both types of common ear infections can cause pain, however, the site of the pain is obviously very different. Most people would be able to tell the difference between outer ear pain (pain on the outer ear or in the ear canal) and the deeper middle ear pain. The different sites of pain can be handy to let you know what you are dealing with.
Ear infections and hearing aids
Infections can be problematic for aid wearers. Swelling in the ear can stop your hearing aid from fitting properly, it can also reduce what you can hear and temporarily change the acoustics of your ear. Steve has had quite a few infections over the years and he says his hearing is usually reduced for the few days that the infection lasts.
He got his first ear infection during his honeymoon in the Dominican Republic (“it was a nice wedding present that stayed with me for a long time”). The initial infection was quite severe and he had to visit the local medical center for antibiotics, which luckily cleared it up quickly. It was a brief swim in the sea that gave him the infection.
After that he started to get recurring infections every three months or so – this lasted for a couple of years and it wasn’t until he bought myself a new pair of aids that the infections finally stopped. He said, “that may have been coincidence but it seemed as though the bacteria causing the infection lived on my aid’s shell and re-infected my ear every so often and wearing new aids finally stopped it”.
Getting rid of a minor infection if you wear hearing aids
If you wear hearing aids and you get an ear infection:
- Try and let your ears get as much air as possible. Try and take your aids out a bit more often and let your ears breath. Particularly true if you wear a moulded in-the-ear model of hearing aid that is stopping air getting into your ear and making it sweaty – that’s a great environment for bacteria to thrive.
- Don’t get your ears wet. That’s advice from the doctor in the Dominican Republic that has stayed with me ever since. Resist the urge to wash your infected ears out. Keep them as dry as possible while infected.
- Wipe your hearing aids after taking them out.
- If the infection lasts more than 4-5 days then go see your doctor or get some ear-drops or antibiotics. The cause of the infection will determine the treatment – you can’t treat a viral infection with antibiotics, for example.
Middle Ear Infection, Otitis Media
What is a middle ear infection?
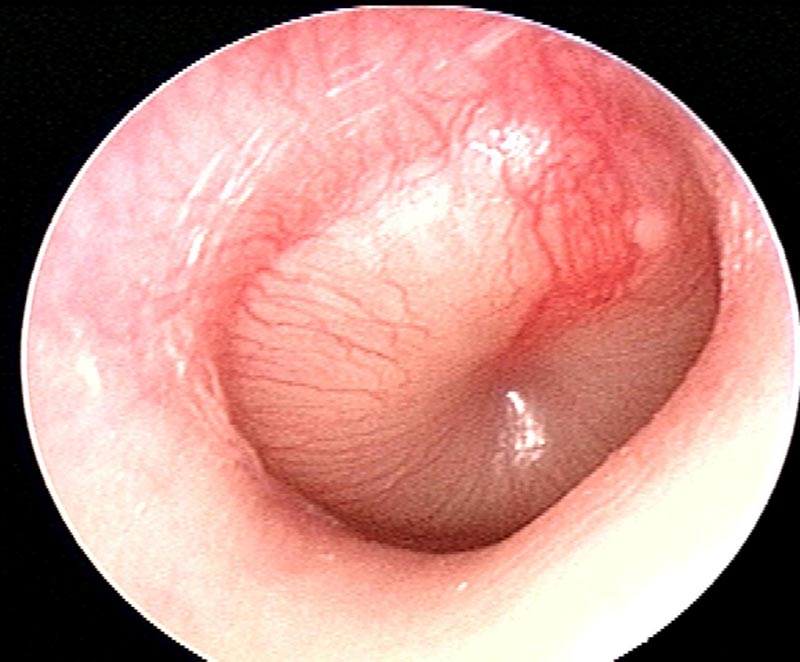
Middle ear infections or otitis media occur inside the middle ear cavity, behind the eardrum. They happen when a virus or bacteria cause the area behind the eardrum to become inflamed. You can see in the image taken by a video otoscope the eardrum is inflamed and bulging outward. All of the usual physical landmarks on the eardrum have been masked by the thick white fluid that is behind the eardrum.
When an infection gets to this stage there is usually quite a bit of pain and probably a fever. However, That is not always the case. I once saw a lady who was complaining about her hearing aid not working well who had an eardrum that looked a lot like the one in the image. But, she felt no pain whatsoever and suffered no fever, she was completely and astonishingly asymptomatic (without symptoms).
Middle ear infections are widespread in young children but can occur in adults as well. Most children will have a bout of otitis media during their early life even if there are no symptoms. The primary cause for this issue in children is often a combination of upper respiratory tract infection and eustachian tube dysfunction. The eustachian tube connects the middle ear and the back of the nose and throat. It is responsible for drainage and keeping the pressure in the middle ear equal. In children, the eustachian tube is smaller and more horizontal than adults.
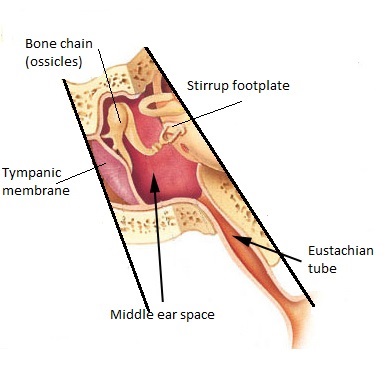
The Eustachian tube is narrow, it also has an isthmus, means an even tighter bit. Mucous membrane (the same as your nose), line the middle ear cavity and the eustachian tube. When you combine all these things with an infection, you get a closed-up eustachian tube, pressure and fluid build up in the middle ear and if the mucous build up gets infected, you get pain. Most middle ear infections occur during the winter and early spring. Quite often, middle ear infections will go away without any medication. However, if the pain persists or you develop a fever, you should seek medical treatment.
What are the types of middle ear infections?
There are two types of middle ear infections, the medical terms for them are, acute otitis media and otitis media with effusion. Let me explain the difference:
- Acute otitis media: Acute otitis media usually comes on quickly, it is normally accompanied by fever and ear pain. A hearing impairment can often occur as a result of trapped fluid and/or mucous in the middle ear cavity.
- Otitis media with effusion: Otitis media with effusion is slightly different. After a mid-ear infection is treated, sometimes mucous and fluid will continue to build up in the middle ear. This fluid isn’t infected, however, it can cause the feeling of the ear being full and affect your ability to hear clearly.
What causes a middle ear infection?
There are a number of reasons why someone can get middle ear infections. More often than not, a respiratory tract infection spreads to the ears through the eustachian tube. When that happens, the tube can become inflamed and blocked, naturally occurring fluid will collect behind the eardrum. If bacteria grow in the fluid, it will inflame the entire middle ear cavity causing pain and infection.
What are the symptoms of a middle ear infection?
The symptoms of middle ear infection are:
- Pain
- Fever
- Pressure or fullness in the ear
- For a child, tugging or pulling at the ear
- Hearing loss
- Puss or fluid draining from the ear canal
- Headaches
Diagnosing middle ear infections
In general, the diagnosis of mid-ear infections is undertaken by using an otoscope to view the ear canal and eardrum. We are looking for redness, swelling, or signs of pus or fluid in the ear canal. If we can see the eardrum, we are looking for signs of fluid build-up behind it. We can also diagnose mid-ear infections with a test called tympanometry. Tympanometry checks the function of the middle ear and it is a simple, quick and effective test procedure.
Treating middle ear infections
Many middle ear infections are treated with antibiotics. In most cases, the antibiotics will be taken orally. On some occasion, antibiotic ear drops may be prescribed. They will also prescribe pain medication or advise the use of over-the-counter pain relievers. Many Doctors will also advise the use of a decongestant, nasal steroids, or an antihistamine.
Opening The Eustachian Tubes
A helpful technique here can be popping your ears, the medical term is auto-insufflation. It is a technique taught to scuba divers to equalise pressure, and it also is a favourite of anyone who flies regularly. It’s meant to help clear your eustachian tubes. You do this by squeezing your nose, closing your mouth, and very gently exhaling. This can send air into the eustachian tubes, causing them to open, relieving pressure and help drain the fluid. Be careful doing this, if your middle ears are well and truly infected this can be painful.
What are the complications associated with middle ear infections?
While complications are rare, they do sometimes occur, especially if someone suffers from a chronic mid-ear infection. complications associated with middle ear infections are:
- An infection that spreads to the bones of the ear
- An infection that spreads to the fluid around the brain and spinal cord (what caused the death of Andrew Broadhurst)
- Permanent hearing loss
- Perforated (ruptured) eardrums
Otitis Externa, Outer Ear Infection
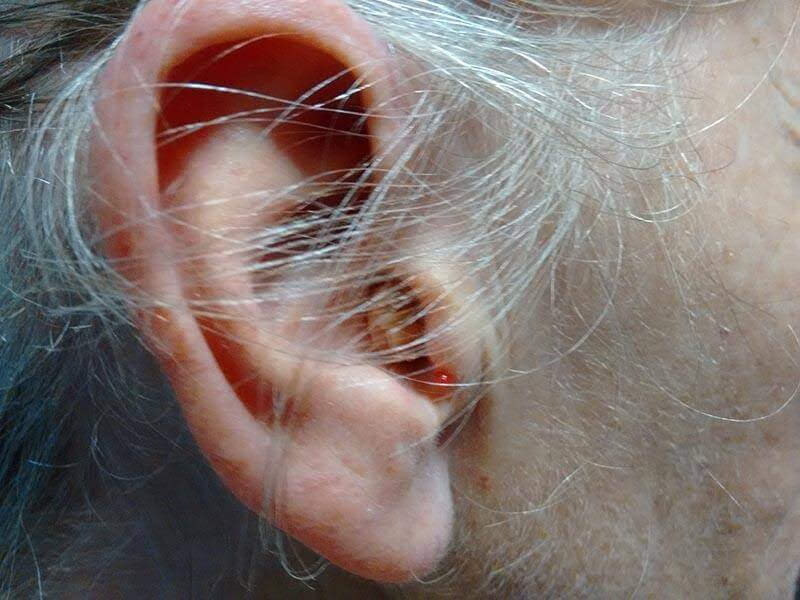
Sometimes this type of infection is called “Swimmer’s Ear”, it is an infection of the eardrum, ear canal or outer ear. The reason it is often referred to as swimmer’s ear is that it is often caused by swimming. It often begins with water inside the ear canal, however, other things can cause it. In general, many outer ear infections are fungal in nature, but I have seen some whopping bacterial ones. While both types of ear infections can cause pain and discomfort, outer ear infections affect the visible part of the ear and canal, often appearing as swelling, redness and itchiness. Symptoms of outer ear infection:
- Painful ear
- Often tender to touch
- Occasionally pus or fluid
- Red appearance
- Swollen
Treating outer ear infections
First off, the outer ear should be carefully cleaned. That is then followed by the application of antibacterial or antifungal and anti-inflammatory medications on your ear. Antibiotics would be prescribed if your doctor thinks the infection is bacterial. Viral is different and irritating, viral infections don’t really have a treatment, simply clean it and put antibacterial medication on it so that it doesn’t turn bacterial. You then just have to wait for the infection to sort itself out. However, if it is something like herpes simplex (don’t panic, it’s a cold sore), more specialised treatment may be necessary.
Preventing Future Infections
There are a couple of things you can do to prevent a further infection, especially in the case of outer ear infection. Here is what you can do:
- Don’t stick anything in your damned ear, no fingers, no bobby pins, no keys, nothing, de nada
- Try to keep water out of your ears. If you’re a frequent swimmer, get earplugs or a swimming cap
- If you didn’t follow the rule above (idiot) shake out or drain any trapped water inside your ears once you get out of a pool or ocean.
- If you are suffering from a bad cold, use a decongestant, this can help keep the eustachian tubes open
- If you feel stuffed up, try clearing your eustachian tubes by auto-insufflation